Brave New World In Veterinary Medicine
by Veterinary Practice News Editors | November 30, 2011 12:11 pm
North Carolina State University is the only university in the country to offer autologous bone marrow transplants (BMT) for dogs with lymphoma—one of the most common canine cancers.
Steven Suter, VMD, MS, Ph.D., Dipl. ACVIM (Oncology), an assistant professor of oncology at North Carolina State University, has been performing the transplants since October 2008. He says that a 40-50 percent cure rate is reported in humans with B-cell lymphoma using the same procedure, although the canine data is still tentative.
“When do you say a dog is cured?” Dr. Suter asks. “For people it is five years out [after the transplant procedure]. For dogs I estimate we can say two years after treatment is a success. In the first group of 24 dogs with B-cell lymphoma that we treated, eight are long-term survivors.”
Suter started providing this service with the hope that the procedure could be perfected and performed in the specialty clinical setting. Since the inception of the project, Suter has continued to modify the protocol.
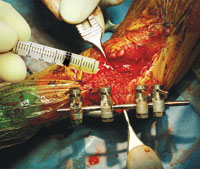
Apply: The rehydrated graft is applied into a surgery site. If a surgery site is not very vascular, pre-mixing with patient blood is advised.
“We now use a much higher dose of Cytoxan, which is given at 750 mg/kg,” Suter says. “This procedure is an alternative to half-body radiation. After diagnosis with lymphoma by the patient’s oncologist, chemotherapy will induce a clinical remission. This is then followed by high-dose Cytoxan, which is given by the local oncologist.
“The patient then comes to NC State, where tests are performed to confirm remission,” Suter continues. “We give subcutaneous doses of Neupogen, a human drug that drives CD34+ progenitor cells [also called bone marrow stem cells] from the bone marrow into the peripheral blood. The patient is connected to an apheresis machine and the bone marrow stem cells are harvested.
Ortho Before: A radius ulna re-fracture in an osteopenic dog.
“The collected cells are refrigerated while the patient undergoes 11Gy of total body radiation over a period of two days,” Suter says. “Immediately after TBI, the stem cells are infused into the patient via an IV catheter. The infused cells then start producing new, healthy peripheral blood cells in approximately two weeks.”
Patients are kept in an isolation ward when their neutrophil count is less than 1,000/µ and kept in the intensive care unit when their platelets are less than 10,000/µ. Once these values normalize, the patients are ready to go home.
Allogeneic BMT—where stem cells are harvested from a genetically similar donor—is uncommon in veterinary medicine because no canine bone marrow registries exist and owners rarely know or have access to relatives of their pets.
.jpg)
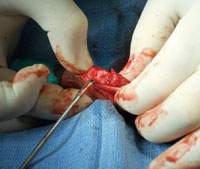
Ortho Apply: The orthopedic bone graft being applied to the fracture site.
The apheresis machine costs between $60,000 and $80,000 and the procedure comes with a $15,000 price tag, making the procedure costly to both the practitioner and client.
Suter wants to educate owners and veterinarians about the viability of the procedure. If performed more frequently, its expense could eventually be reduced.
Suter continues to modify the protocol in hopes of both decreasing expenses and increasing the cure rate. He plans to publish his results as they are finalized.
****
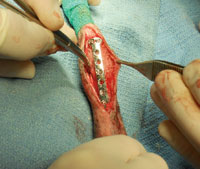
Ortho Applied: The grafted site is ready to be sutured closed.
Allograft bone banking has been available in human medicine for decades, so many human tissue banks exist. But only Veterinary Transplant Services of Kent, Wash., provides animal bone allograft, tissue that comes from another individual of the same species.
VTS was established in 1996, originally focused on assisting veterinary orthopedic surgeons. It has since expanded to provide products used by primary care practitioners, veterinary dentists and oral surgeons.
The company provides bone, soft tissue and cornea allografts for transplantation into animals.
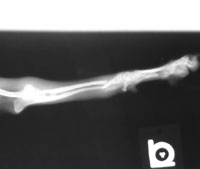
Ortho X-Ray Before: The re-fractured radius and ulna.
“About 90 percent of the veterinary schools use allograft today, so new graduates will be accustomed to using biological material,” says Helen Newman, Ph.D., founder and director of VTS. “We’ve seen a steady transition toward using biological material in the industry.”
The company serves an international audience. Vacuum-sealed packaging maintains product integrity for five years. Freeze-dried products can be shipped at room temperature and frozen products are shipped on dry ice. Freeze-dried products are rehydrated upon use with saline or patient blood.
The company carries products for feline, canine and equine patients.
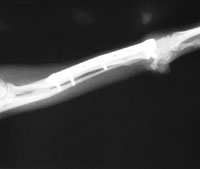
Ortho X-Ray After(10 weeks): The fracture is fully healed. The patient is weight-bearing and happy.
“With the various processes these materials undergo, we can create optimal size ranges for our particulate allograft products,” Newman says. “We also have virtually eliminated the possibility of infection or rejection in the patient, because all grafts meet USP guidelines for sterility, viable cells are removed, and freeze-dried grafts are sterilized by gamma irradiation.”
A new product, Ossiflex Bone Membrane, can help repair oronasal fistulas, cleft palates and cranio-facial defects as well as guided bone regeneration and fracture bridging.
Dental Use
Judith Yee, DVM, Dipl. AVDC, of Desert Veterinary Specialists in Palm Desert, Calif., says she has used Ossiflex to repair cleft palates, in fractures and in cases where bone loss has occurred.
“Sometimes bone loss can be so severe that I have to extract the affected tooth,” Dr. Yee says. “There are cases, though, where we can actually save teeth from extraction by using Osteoallograft Periomix to provide faster bone regeneration. ... Having this service option in the profession is really good for enhancing the standard of care for patients and for the industry.”
The product is made of osteoinductive demineralized bone matrix (DBM) and osteoconductive cancellous bone chips.
With greater awareness of animals’ dental issues—specifically periodontal disease, Osteoallograft Periomix has become a tool in specialized and general dental applications.
“The product comes in different particulate sizes, for different needs and patient accommodation,” says Rocco Mele, DVM, of Eastpoint Pet Clinic, P.C. in Tucson, Ariz. “I don’t do extractions without it. When the product is used, it provides a greater quality of bone, which is ideal for dental implants—or just for reducing swelling and pain post-surgically.”
Dr. Mele says he also uses the product for feline patients suffering from feline resorptive disease.
“When a cat has many teeth pulled all at once, sockets are exposed, which are uncomfortable. It makes the animal vulnerable to infection and [the sockets] are very painful,” Mele says. “Filling sockets with the grafting material eases and speeds the bone regrowth.”
Using the material for preservation of teeth (by preventing horizontal and vertical bone loss), it also serves a mental health purpose, Newman says.
“Dogs like to chew toys, which provides a psychological release,” Newman says. “When numerous teeth are pulled, dogs sometimes develop compulsive habits like licking. Bone grafts, when packed into pockets of bone loss around teeth, can help re-anchor teeth so dogs can continue to get satisfaction from chewing their toys.”
Orthopedic Use
Using bone allografts means the veterinarian doesn’t need to procure graft material from the patient’s own bone, which has its own associated pain and risks. The company’s allograft provides an osteoconductive scaffold and native, osteoinductive growth factors for faster and stronger bone healing compared with using bone substitutes.
Bone substitutes are inactive, while allografts preserve the body’s naturally occurring growth factors which help accelerate biological fusion, proponents say.
“My business partner is an orthopedic surgeon,” Yee says. “When he needs to repair a delicate bone in a Yorkshire terrier, for example, he uses Orthomix Ultra Fine, which has the same particle size as the Periomix, which I use in my dental cases. The product allows for immediate access to BMPs when it’s placed into the surgery site. This results in an immediate beginning of the healing process. He’s been using these products for about 10 years and I’ve been using them for about six years.”
Yee says using bone allograft compared to using synthetic products is like “comparing apples to oranges.”
“All of the new data discussing use of grafting material is on biological products. Some veterinarians stick with synthetic products because they are comfortable and used to using it, but I would never use synthetic at this point.”
VTS’s technical staff comprises certified tissue banking specialists and its advisory board includes biologists and board certified veterinary surgeons and pathologists. Newman says standards set for human tissue banking facilities are either met or surpassed in all areas of the company’s focus.
The company acquires donors through local emergency clinics and general practices after an animal’s owner has chosen euthanasia. Only after the pet owner has made the decision for euthanasia does the practice introduce the idea of tissue donation to the client.
“We never get involved with the owner’s decision-making for euthanasia because we do not in any way want to influence the owners’ very personal decision about euthanizing their pets,” Newman says. The option of being able to help other animals through tissue donation often helps owners feel a little better about their own loss.”
Source URL: https://www.veterinarypracticenews.com/brave-new-world-in-veterinary-medicine/