Diabetes and dental disease
by Sarah Said | August 16, 2018 12:43 pm
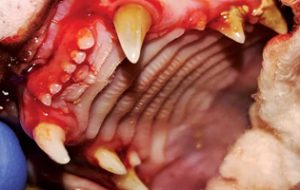
As veterinary practitioners, we see our fair share of diabetic patients who require extensive dental work. The goal with these patients is to improve their quality of life and, in some cases, improve glycemic control by removing a source of chronic infection in the form of periodontal disease. The challenge is to "do no harm" in the process. Invariably, oral surgery will set back the appetite of any patient. Lack of appetite becomes a bigger issue when a patient has diabetes and is supplemented with injectable insulin.
Patients with diabetes are susceptible to developing infections, as high blood sugar levels can weaken immune defenses. In addition, some diabetes-related health issues, such as nerve damage and reduced blood flow to the extremities, increase the body's vulnerability to infection.
Conversely, ongoing chronic infection affects the body's ability to maintain glycemic control. Endogenous hormones produced in response to infection can cause insulin resistance and hyperglycemia. Patients with diabetes may require larger amounts of injectable insulin to keep blood glucose in an acceptable range.
Periodontal disease is the most common oral disease in diabetic dogs and cats. When periodontal disease occurs in diabetic patients, it often seems more severe when compared to age-matched nondiabetic counterparts. This may be due in part to findings of a study of experimentally induced diabetes in dogs. Inflammatory reactions of the gingiva of five beagle dogs were studied in connection with the development of dental plaque. Diabetic dogs showed a lack of typical increase in gingival crevicular fluid and crevicular leukocytes in response to plaque accumulation. This might reflect an impaired defense mechanism, predisposing to a development of pathological changes in the periodontium.1
Preop, intraop, and postop diabetic patients
How do we deal with the diabetic patient preoperatively, intraoperatively, as well as postoperatively? Preoperatively, I typically recommend a fasting period by removing access to food somewhere in the range of 10 p.m. to midnight, with access to water throughout the night. For patients who are receiving long-acting subcutaneous injectable insulin every 12 hours, I usually recommend the patient receive a half dose of the usual morning dose. I try to schedule my diabetic patients as the first cases of the day whenever possible. Bloodwork on the morning of the procedure (in addition to a full CBC/chemistry/T4 done within weeks of the procedure) may consist of a blood glucose level, electrolytes, venous pH, hematocrit, BUN, and creatinine. Depending on what the morning's blood glucose level showed, I might repeat a blood glucose test once again during the procedure and every few hours postoperatively to assess how to adjust the afternoon/evening dose of insulin. An intraoperative intravenous dose of ampicillin or clindamycin may be warranted.
Nonsalvageable teeth are extracted. These sites are debrided, lavaged, and closed with absorbable monofilament suture. Teeth that can be saved are treated with subgingival cleaning and polishing +/- open or closed root planing and local delivery of periodontal antibiotic. Extractions will cause a transient decrease in appetite when compared to preoperative appetite, but after a brief recuperative period, the appetite will return to normal and sometimes better than normal.
I generally keep my diabetic patients overnight if they've had significant oral surgery for serial glucose monitoring, intravenous opioid administration, possible intravenous antibiotic administration, and assessment of appetite on the morning after surgery. Occasionally, I will send a diabetic cat home on the day of the procedure if I feel that the patient is too stressed and will do better at home.
During the postoperative period, close attention to food intake is critical. Excessive insulin supplementation in the face of a faltering appetite may result in hypoglycemia. Lack of insulin supplementation may result in ketoacidosis. When glucose is unable to enter cells due to lack of insulin, the body breaks down fat as an alternative energy source, releasing free fatty acids into the bloodstream. The liver subsequently converts FFAs to triglycerides and ketone bodies. Predisposing diseases and exposure to stressful situations (e.g. hospitalization and oral surgery) also can lead to ketoacidosis in the absence of appropriate insulin supplementation.
To increase the chances of an uncomplicated recovery, oral surgery should be efficient and effective in removing any source of oral pain. A case report in the Journal of Veterinary Dentistry described complications associated with poorly performed extractions in a diabetic cat.2 The cat presented 10 days after a previous dental procedure with ketoacidosis and possible thromboembolism. During a second dental procedure, 22 retained tooth roots were removed. After nearly two weeks in the hospital, the cat was doing well enough to be discharged from the hospital.
Do diabetic cats and dogs heal less well after oral surgery? It may depend at least in part on the level of glycemic control of the individual patient, but I personally do not see an increased likelihood of dehiscence of oral surgery sites in diabetic patients compared to nondiabetic patients. However,
I do use simple interrupted suture patterns for both diabetics and nondiabetics, so this may help decrease dehiscence over continuous patterns. The mouth has an excellent blood supply and tends to heal rapidly, even in diabetic patients.
| 7 phrases that can kill dental compliance |
| By Wendy S. Myers, CVJ
1) "Here's the estimate for your pet's dental procedure." 2) "I recommend you get your dog's teeth cleaned." 3) "Let's think about cleaning your pet's teeth." 4) "You should consider brushing your pet's teeth." 5) "Let's watch it for now." 6) "I see a little tartar on your cat's teeth." 7) "Let's wait until February." Wendy S. Myers, CVJ, owns Communication Solutions for Veterinarians in Castle Pines, Colo., and offers consulting, seminars, and monthly CE credit webinars. Reach her at wmyers@csvets.com or csvets.com. For more training on dental compliance, order my one-hour webinar, "How to Get to Yes for Dentistry," which includes unlimited playback, a handout, one hour of CE credit, and a CE certificate, visit bit.ly/2yWlatv. |
References
1 Matsson L, Attstrom R, Granath L. Inflammatory reactions in the gingival region during the development of bacterial plaque in alloxan-diabetic dogs. J Periodontal Res. 1980;15(5):516-24.
2 Reiter AM, Brady CA, Harvey CE. Local and systemic complications in a cat after poorly performed dental extractions. J Vet Dent. 2004;21(4):215-21.
Dr. John Lewis practices veterinary dentistry and oral surgery at NorthStar Vets in Robbinsville, N.J.
Source URL: https://www.veterinarypracticenews.com/diabetes-and-dental-disease/